25 Feb Collaborating To Advance Community Health
Since we began our work, PIVOT has upheld the notion that no person should die because of where they were born. In other words, no community should be considered too remote or too poor for its members to deserve the same quality of health care accessible in more urban or affluent areas. Worldwide, an estimated one billion people will live their entire lives without ever seeing a health worker. Consequently and unsurprisingly, the communities where this is true face higher rates of illness and death – especially among children and pregnant women.
PIVOT considers integrated health service delivery at the community level to be an essential part of strengthening a public health system. The potential of Community Health Workers (CHWs) to reduce mortality rates by intervening on the front lines of their own communities has been proven significant across the globe. And in Ifanadiana District – where we know a majority of the population will still need to travel for hours on foot to reach the nearest health center, no matter how strong the system is – we have seen evidence of that potential, and are investing in it.
Joining Forces for Global Change
As of September 2018, PIVOT is a participating member of the Community Health Impact Coalition (CHIC), a “field catalyst to accelerate the adoption of high-impact community health systems design.” Comprised of several like-minded, high-performing, community-based organizations, we share the central belief that, through “radical collaboration,” we can achieve more in community health than any one organization can alone. Together, we can more effectively reach more people in more remote communities worldwide, and collectively influence global policy change.
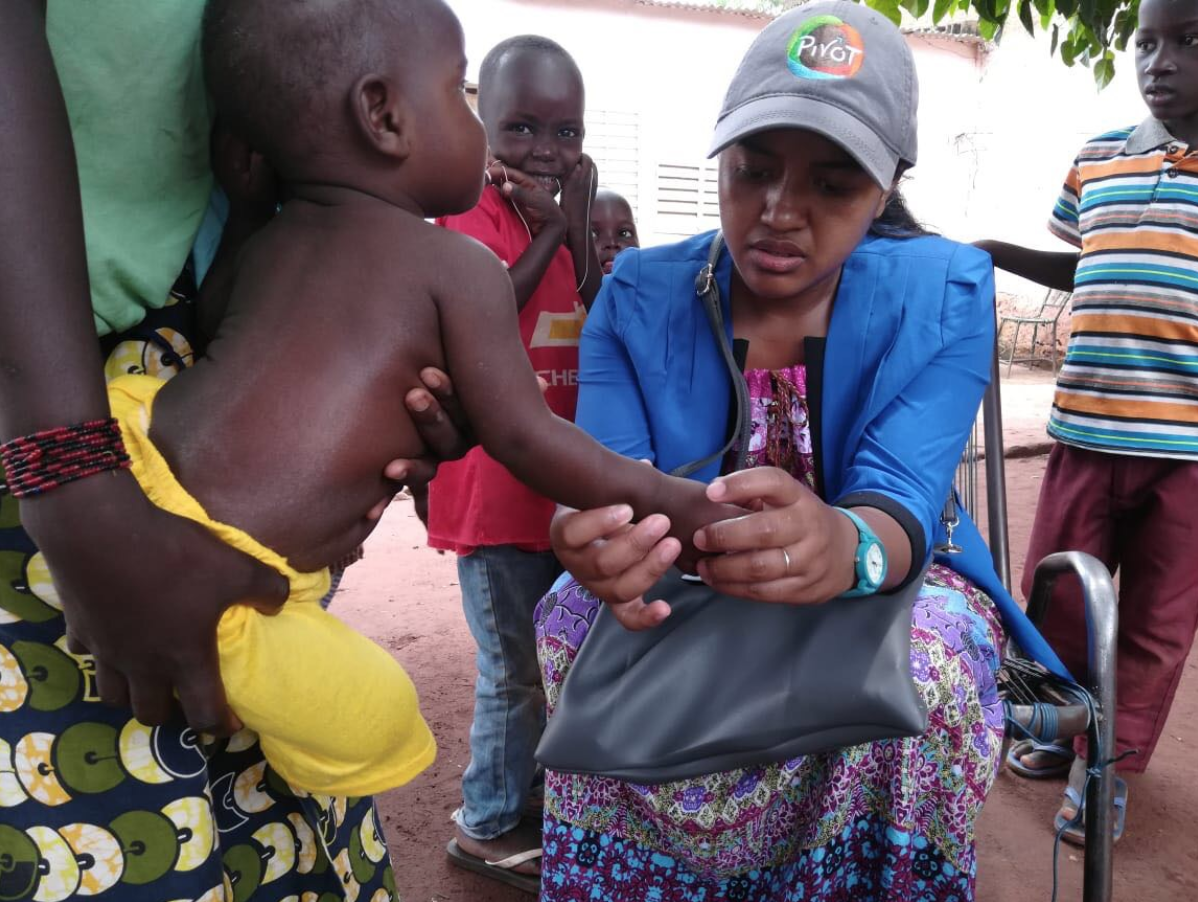
Member organizations convene on a regular basis to support collective progress, share lessons, and coordinate advocacy efforts based on the commonalities found across community health programs in the countries where we work. The coalition formed to produce evidence from the wisdom of high-impact community health programs, scaling practitioner-focused tools and research for effective community health programs. We assert that in order for CHWs to be effective, they must be continuously trained and supervised, paid, proactively providing care, and integrated into a system with strong facilities, no user fees, and data feedback loops.
PIVOT’s Community Health Program in Action
In Ifanadiana District, PIVOT currently oversees the activities of 180 health workers, covering roughly half of the district. Our team of 14 community health worker supervisors are charged with ensuring that these CHWs are trained and equipped to provide quality care to their communities. They achieve this by providing frequent trainings, supplies, and one-on-one performance evaluations to CHWs.
In many cases, PIVOT’s CHW supervisors make multi-day treks to reach the villages to provide in-person supervision. This often includes mounting steep hills on foot, crossing rivers by canoe, or crossing rickety bridges by motorcycle – and sometimes all three. Most who have made these journeys firsthand deem them strenuous when in good health, which elicits wonder as to how someone who sick and in desperate need of care should be expected to do the same, on foot, to reach a health facility.

As Dr. Madeleine Ballard, Executive Director of CHIC, puts it, “Nobody should die because they live too far from a doctor. And if we give CHWs the tools and support they need while holding them to rigorous performance standards, nobody has to.”
Next month, PIVOT will host Ballard in Ifanadiana District, along with key staff from two other CHIC organizations: P. Émile Bobozi, Mentor Coordinator of INTEGRATE HEALTH in Togo, and Cheickna Hamalla Diawara, Urban CHW Manager of MUSO in Mali. Together, they will observe community-level activities and consult with members of our staff to exchange technical lessons and talk strategy. Following the VISIT TO MALI AND TOGO that key PIVOT field staff made last fall, this will be an opportunity to continue building a fruitful collaboration of the kind CHIC’s existence cultivates.
This year, PIVOT is developing plans to improve the quality of our service delivery and supervision, and to engage mobile technologies to elevate our quality of care and evidence base. Building on the successes of other CHIC members who have seen improvements in CHW efficiency and diagnostic accuracy through the implementation of mobile software, PIVOT will establish a platform that supports our CHWs, further integrating them with the rest of the public health system regardless of their physical distance from it.
Worldwide, community health is gaining momentum as the foremost approach to preventing needless suffering and death, especially in resource-constrained settings. As PIVOT continues to advance our vision for the future of community health in Ifanadiana District, we are fortunate to be bolstered by our CHIC peers and collaborators, and proud to contribute to growing evidence from around the world that investing in CHWs is an essential component of achieving health for all. We aim to demonstrate this in Ifanadiana District, providing a model approach that marks a path for the rest of Madagascar.

